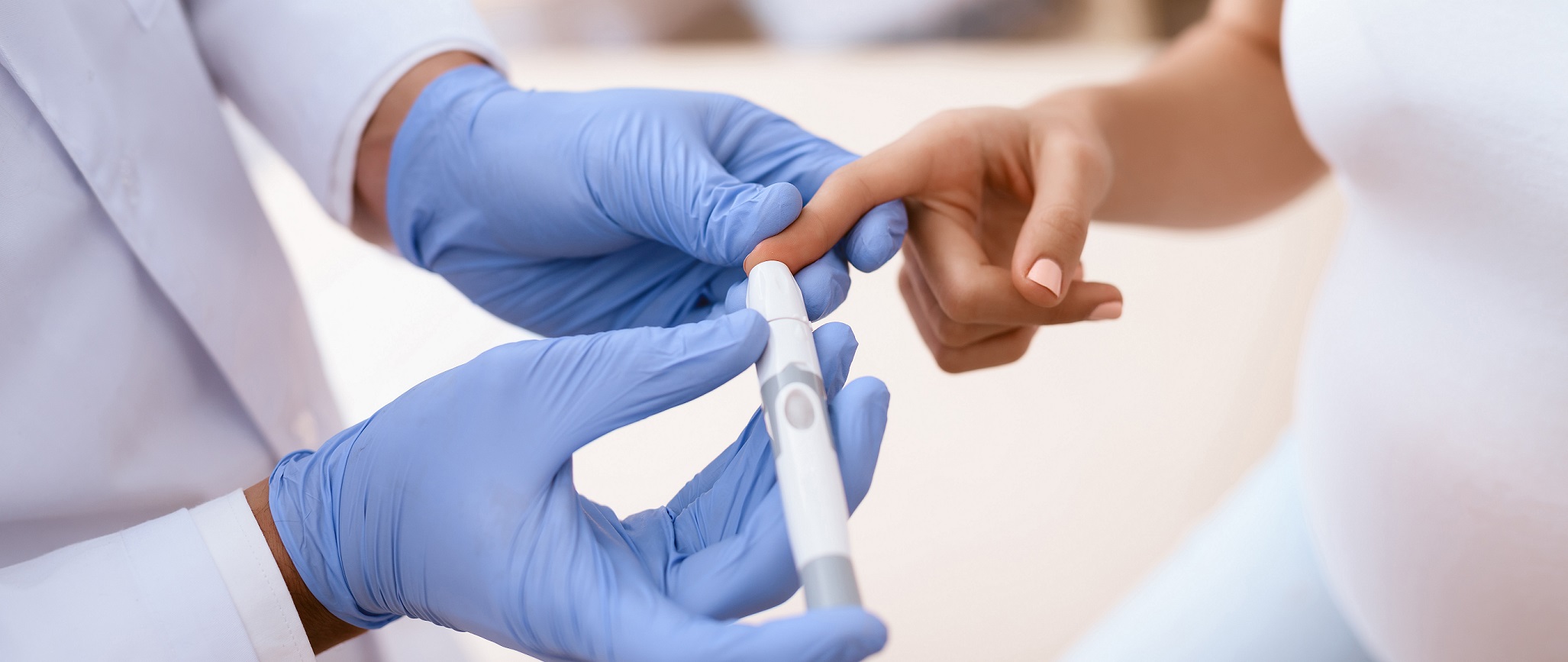
Gestational diabetes is a diabetes that has occurred during pregnancy. As with other types of diabetes, the ability of glucose to enter the cells is impaired, which means that it can’t be converted into energy. These changes lead to an increase in blood sugar — a deviation that has a negative effect on the mother and baby. Although potentially dangerous, gestational diabetes can be controlled and complications can be prevented.
WHAT ARE THE RISK FACTORS?
Although the mechanisms by which gestational diabetes occurs are not yet fully understood, some risk factors are known. These include being overweight, polycystic ovarian syndrome and genetic predisposition (relatives with diabetes).
At the first visit, your obstetrician-gynecologist will assess whether you fall into any of the risk groups for gestational diabetes. You will be given blood and urine tests according to the current Maternal Health program.
If you do not have risk factors, you will be offered a prophylactic test for diabetes in the second trimester of pregnancy — between the 24th and 28th week of gestation.
WHAT ARE THE SYMPTOMS OF GESTATIONAL DIABETES?
Diabetes is often asymptomatic for a long time. Gestational diabetes usually occurs around the second or third trimester. The symptoms are non-specific — thirst, fatigue, dry mouth, frequent urination — all unpleasant sensations that happen in a normal pregnancy.
WHAT ARE THE RISKS FOR MY BABY?
The most common risks are:
- Large fetus (fetal macrosomia) — due to high blood sugar levels and insulin resistance in pregnant women with gestational diabetes, more blood sugar passes through the placenta and stimulates the baby’s pancreas to produce more insulin. As a result of the altered balance, the baby gains more muscle mass, subcutaneous fat and larger internal organs. In turn, this leads to birth traumas.
- Hypoglycemia (low blood sugar) of the newborn
- Premature birth
- Prolonged jaundice
- Risk of developing type 2 diabetes in the future.
DIABETES CONTROL
To minimize the risks, it is extremely important to start treatment immediately after the diagnosis of gestational diabetes. You will be prescribed a diet and a medication that controls your blood sugar levels — tablets or an insulin pen. You will also need to measure your blood sugar regularly with a glucometer.
Daily walks and light workouts help to normalize blood sugar, and also have other positive effects — improve mood and self-esteem and are associated with easier recovery after birth.
PROGNOSIS
Women with gestational diabetes usually normalize their blood sugar levels 6-12 weeks after giving birth. They are more likely to develop gestational diabetes again during a second pregnancy. They are also prone to developing type 2 diabetes in the future, so it is highly recommended that you get tested (oral glucose tolerance test) every 2 years.
In early diagnosed gestational diabetes, the prognosis for mother and baby is really positive. Share with your supervising obstetrician-gynecologist your complaints, no matter how minimal they may seem to you — timely measures are always preferable to treating the consequences.